Wearable Technologies and AI in Asthma Management: A Literature Review on Adherence Challenges and Innovations in Asthma Care
DOI:
https://doi.org/10.31033/IJEMR/16.1.2026.1843Keywords:
Asthma Management, Wearable Respiratory Monitoring, Inhaler Adherence, Artificial Intelligence, Machine Learning, Real-Time Drug Delivery, Mobile Health Applications, Contactless Monitoring, Inhalers, Smart Medication TrackingAbstract
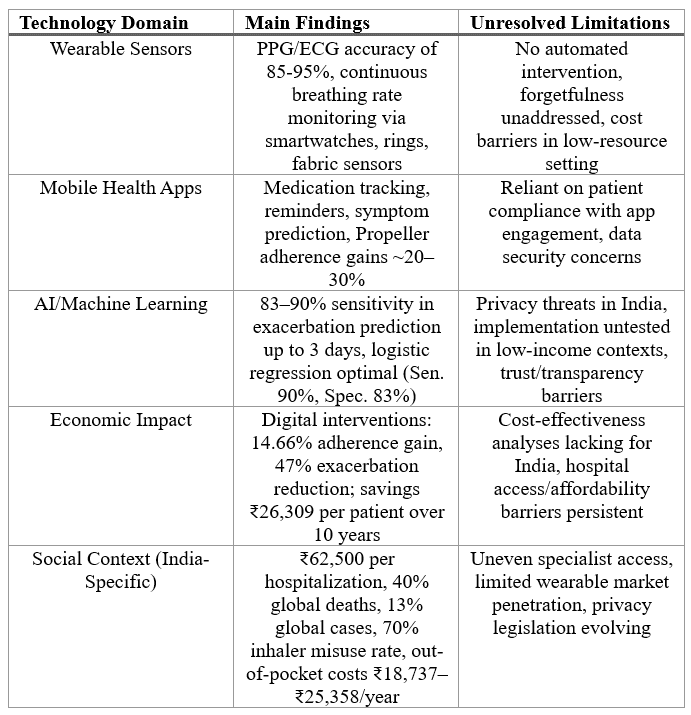
Asthma is among the most critical global health disorder affecting around 260 million individuals worldwide with significant mortality rates, particularly in India where it accounts for over 40% of global asthma deaths despite representing only 13% cases of the world. A fundamental challenge in asthma management arises from inhaler misuse, forgetfulness of inhaler, and absence of real-time monitoring integrated with drug delivery. This literature review examines emerging technologies in asthma management with a focus on wearable sensors, contactless monitoring systems, artificial intelligence (AI), machine learning (ML) applications and real-time drug delivery. A comprehensive examination of published literature reveals that while digital health interventions, including mobile health applications (SaniQ Asthma, Propeller), wearable vital signs monitoring (ECG, PPG sensors in smartwatches and rings), and predictive AI algorithms have demonstrated measurable improvements in medication adherence (14–47% gains) and exacerbation prediction (83–90% sensitivity), critical gaps still persist. Specifically, no integrated system currently combines real-time respiratory monitoring with automated drug delivery mechanisms, and implementation barriers in low-resource settings remain underexplored. Additionally, inhaler misuse affects 70% of patients globally, forgetfulness of inhalers contributes to emergency hospitalizations averaging ₹62,500 in India, and privacy concerns threaten AI adoption. This review identifies key literature-derived principles like continuous wrist-worn monitoring, predictive algorithms, and mobile integration that may address persistent accessibility and adherence barriers. Future research must prioritize cost-effectiveness analyses, data security frameworks, and implementation strategies tailored to India's out-of-pocket cost constraints and specialist access inequalities. These efforts are essential for reframing asthma care from reactive symptom management to proactive, equitable intervention.
Downloads
References
Barnes, P. J. (2017). Cellular and molecular mechanisms of asthma and COPD. Clinical Science, 131(13), 1541–1558. https://doi.org/10.1042/CS20160487
World Health Organization. (2024, May 6). Asthma fact sheet. https://www.who.int/news-room/fact-sheets/detail/asthma
Global Initiative for Asthma. (2021). Global strategy for asthma management and prevention. https://ginasthma.org/wp-content/uploads/2021/05/GINA-Main-Report-2021-V2-WMS.pdf
Nair, P., Madan, K., Mohan, A., Guleria, R., & Kant, S. (2022). Asthma in India: Needs, gaps and opportunities. Lung India, 39(4), 335–342. https://doi.org/10.4103/lungindia.lungindia_273_21
Global Asthma Network. (2023). Global asthma report 2023: Burden of asthma. https://globalasthmareport.org/burden/burden.php
Finkelstein, J., & Jeong, I. C. (2017). Machine learning approaches to personalize early prediction of asthma exacerbations. Annals of the New York Academy of Sciences, 1387(1), 153–165. https://doi.org/10.1111/nyas.13218
Taylor, L., Ding, X., Clifton, D., & Lu, H. (2020). Wearable vital signs monitoring for patients with asthma: A review. IEEE Sensors Journal, 22(3), 1734–1751. https://doi.org/10.1109/JSEN.2022.3224411
British Lung Foundation. (2021, July 4). SaniQ Asthma—Pollen and asthma. https://www.blf.org.uk/technology-for-lung-health/saniq-asthma-pollen-asthma
Propeller Health. (2021, August 6). Meet Propeller: The doctor-recommended way to manage your asthma or COPD. https://propellerhealth.com
Smart Asthma. (2021, August 5). Asthma control in your pocket. https://smartasthma.com
Baños, O., Villalonga, C., Damas, M., Gloesekoetter, P., Pomares, H., & Rojas, I. (2014). PhysioDroid: Combining wearable health sensors and mobile devices for a ubiquitous, continuous, and personal monitoring. The Scientific World Journal, 2014, Article 490824. https://doi.org/10.1155/2014/490824
Oura. (2021, August 20). Ring and app: The Oura difference. https://ouraring.com/blog/the-oura-difference/
Subbe, C., & Kinsella, S. (2018). Continuous monitoring of respiratory rate in emergency admissions: Evaluation of the RespiraSense sensor in acute care compared to the industry standard and gold standard. Sensors, 18(8), 2700. https://doi.org/10.3390/s18082700
Chu, M., et al. (2019). Respiration rate and volume measurements using wearable strain sensors. NPJ Digital Medicine, 2(1), 1–9. https://doi.org/10.1038/s41746-019-0083-3
BIOPAC. (2022, March 29). BioHarness: Lightweight, portable data logger and telemetry system. https://www.biopac.com/product/bioharness-telemetry-logging-systems/
Çakmaklı, S., Özdemir, A., Frat, H., & Aypak, C. (2023). An evaluation of the use of inhalers in asthma and chronic obstructive pulmonary disease. Journal of Taibah University Medical Sciences, 18(4), 860–867. https://doi.org/10.1016/j.jtumed.2023.01.001
Rogliani, P., Calzetta, L., & Coppola, A. (2017). Optimizing drug delivery in COPD: The role of inhaler devices. Respiratory Medicine, 124, 6–14. https://doi.org/10.1016/j.rmed.2017.01.006
Biddiscombe, M. F., & Usmani, O. S. (2018). Is there room for further innovation in inhaled therapy for airways disease? Breathe, 14(3), 216–224. https://doi.org/10.1183/20734735.020318
Kikidis, D., Votis, K., Tzovaras, D., et al. (2016). The digital asthma patient: The history and future of inhaler-based health monitoring devices. Journal of Aerosol Medicine and Pulmonary Drug Delivery, 29(3), 219–232. https://doi.org/10.1089/jamp.2015.1263
Tan, L. D., Nguyen, N., Lopez, E., Peverini, D., Shedd, M., Alismail, A., & Nguyen, H. B. (2025). Artificial intelligence in the management of asthma: A review of a new frontier in patient care. Journal of Asthma and Allergy, 18, 1179–1191. https://doi.org/10.2147/JAA.S535264
Finkelstein, J., & Jeong, I. C. (2017). Machine learning approaches to personalize early prediction of asthma exacerbations. Annals of the New York Academy of Sciences, 1387(1), 153–165. https://doi.org/10.1111/nyas.13218
Zhang, O., Minku, L. L., & Gonem, S. (2021). Detecting asthma exacerbations using daily home monitoring and machine learning. Journal of Asthma, 58(11), 1518–1527. https://doi.org/10.1080/02770903.2020.1802746
Gudala, M., Ross, M. E. T., Mogalla, S., Lyons, M., Ramaswamy, P., & Roberts, K. (2022). Benefits of, barriers to, and needs for an artificial intelligence-powered medication information voice chatbot for older adults: Interview study with geriatrics experts. JMIR Aging, 5(2), e32169. https://doi.org/10.2196/32169
Jindal, S., Aggarwal, A. N., & Gupta, D. (2017). Economic burden of asthma in India. Indian Journal of Chest Diseases and Allied Sciences, 59(Suppl), S1–S8. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6034365/
Kumar, S., et al. (2017). Economic burden of asthma among patients visiting a private tertiary care hospital in India. Lung India, 34(6), 547–552. https://doi.org/10.4103/lungindia.lungindia_78_17
Van de Hei, S. J., et al. (2023). Long-term cost-effectiveness of digital inhaler adherence monitoring in severe asthma. Journal of Asthma and Allergy, 16, 1325–1338. https://doi.org/10.2147/JAA.S430223
Papadopoulou, K., et al. (2023). Digital interventions to improve adherence to maintenance treatments in asthma: A systematic review and meta-analysis. Clinical & Experimental Allergy, 53(9), 1120–1137. https://doi.org/10.1111/cea.14351
Asamani, J. A., et al. (2021). Balancing equity and efficiency in the allocation of health resources. International Journal for Equity in Health, 20(1), 212. https://doi.org/10.1186/s12939-021-01531-1
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Rushal Nandeshwar, Sanjukta Ghosh

This work is licensed under a Creative Commons Attribution 4.0 International License.
Research Articles in 'International Journal of Engineering and Management Research' are Open Access articles published under the Creative Commons CC BY License Creative Commons Attribution 4.0 International License http://creativecommons.org/licenses/by/4.0/. This license allows you to share – copy and redistribute the material in any medium or format. Adapt – remix, transform, and build upon the material for any purpose, even commercially.









